Diabetes and Kidney Disease: Understanding Diabetic Nephropathy
Diabetes affects many parts of the body, but one of the most serious long-term complications involves the kidneys. Over time, high blood sugar can damage the delicate filtering system within the kidneys, leading to a condition known as Diabetic Nephropathy. This form of kidney damage is one of the leading causes of Chronic Kidney Disease and Kidney Failure worldwide.
The good news is that early detection and proper diabetes management can significantly reduce the risk of kidney complications. By understanding how diabetes affects the kidneys and learning how to protect kidney function, patients can take important steps toward maintaining long-term health.
This article explains what diabetic nephropathy is, why it develops, the warning signs to watch for, and strategies to help prevent or slow kidney damage.
How the Kidneys Work
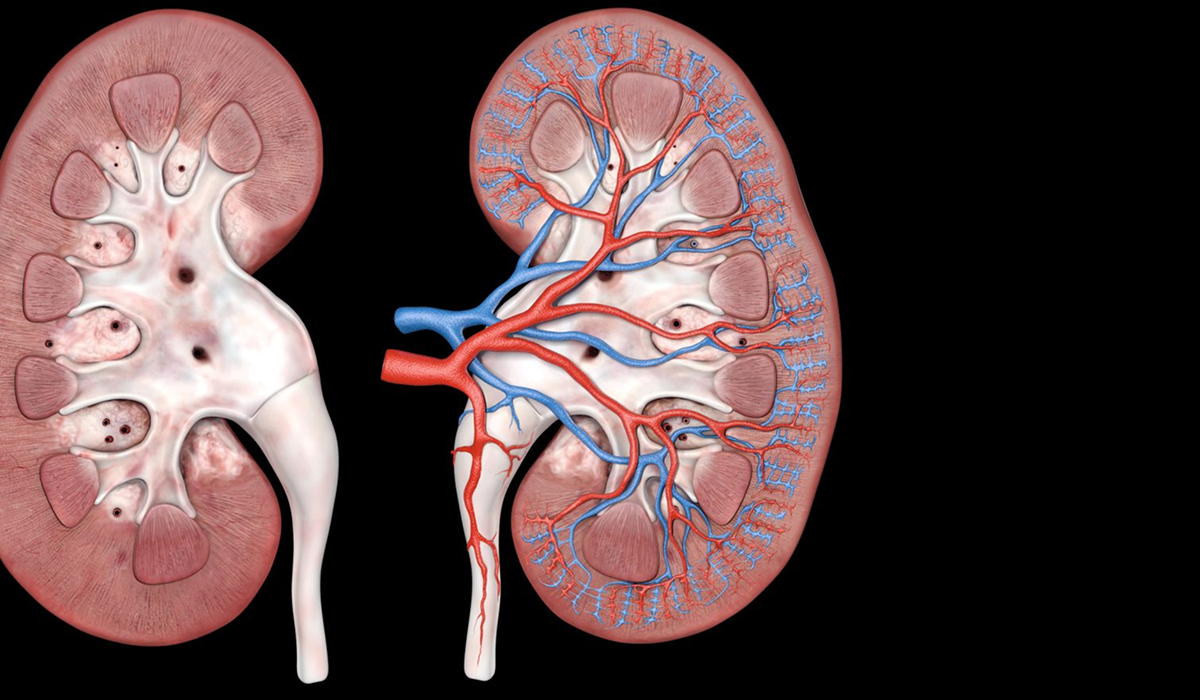
The kidneys are two bean-shaped organs located on either side of the spine. Their primary job is to filter waste products and excess fluids from the blood, which are then removed from the body through urine.
Each kidney contains about one million tiny filtering units called nephrons. Inside these nephrons are clusters of small blood vessels called glomeruli that act as microscopic filters.
When the kidneys are functioning normally, they:
- Remove toxins and waste from the bloodstream
- Maintain proper fluid balance
- Regulate electrolyte levels such as sodium and potassium
- Help control blood pressure
- Produce hormones that support red blood cell production and bone health
However, chronic high blood sugar associated with Diabetes Mellitus can damage these delicate structures over time.
What Is Diabetic Nephropathy?
Diabetic Nephropathy is kidney damage that develops as a complication of diabetes. It occurs when high levels of glucose in the blood gradually injure the tiny blood vessels within the kidneys.
This damage reduces the kidneys’ ability to filter waste effectively. As the disease progresses, protein that should normally remain in the bloodstream begins leaking into the urine.
Both Type 1 Diabetes and Type 2 Diabetes can lead to diabetic nephropathy, although the condition is more commonly associated with type 2 diabetes due to its higher prevalence.
Without proper treatment, diabetic nephropathy can eventually progress to End-Stage Renal Disease, a severe condition in which the kidneys lose nearly all ability to function.
Why Diabetes Damages the Kidneys
Several biological changes contribute to kidney damage in people with diabetes.
High Blood Sugar
Elevated glucose levels place stress on the filtering units of the kidneys. Over time, the glomeruli become thickened and scarred, reducing their ability to filter blood efficiently.
High Blood Pressure
Many individuals with diabetes also develop Hypertension. High blood pressure increases pressure within the kidney’s blood vessels, accelerating damage to the filtering structures.
Inflammation and Oxidative Stress
Chronic inflammation and metabolic changes associated with diabetes can damage kidney tissues and promote the buildup of scar tissue.
Protein Leakage
As kidney filters become damaged, they begin allowing proteins such as albumin to pass into the urine. This condition, known as Albuminuria, is often one of the earliest detectable signs of diabetic kidney disease.
Early Signs and Symptoms
One of the challenges of diabetic nephropathy is that it often develops slowly and may not cause noticeable symptoms in its early stages.
Early kidney damage may only be detected through routine laboratory tests. However, as the condition progresses, symptoms may begin to appear.
Possible signs include:
- Swelling in the feet, ankles, legs, or hands
- Increased need to urinate, especially at night
- Fatigue or weakness
- Nausea or loss of appetite
- Difficulty concentrating
- Foamy or bubbly urine (a sign of excess protein)
Because symptoms often appear only after significant damage has occurred, regular screening is essential for individuals living with diabetes.
Who Is at Higher Risk?
While anyone with diabetes can develop kidney disease, certain factors increase the risk.
Common risk factors include:
- Long duration of diabetes
- Poor blood sugar control
- High blood pressure
- Family history of kidney disease
- Smoking
- High cholesterol levels
- Obesity
According to the National Institute of Diabetes and Digestive and Kidney Diseases, approximately one in three adults with diabetes develops some form of kidney disease.
How Diabetic Kidney Disease Is Diagnosed
Healthcare providers use several tests to detect kidney damage in people with diabetes.
Urine Albumin Test
One of the most important screening tools measures the amount of albumin in the urine. Even small amounts of albumin can indicate early kidney damage.
Blood Creatinine Test
A blood test measuring creatinine levels helps estimate how well the kidneys are filtering waste. These results are used to calculate the Estimated Glomerular Filtration Rate (eGFR), which indicates overall kidney function.
Blood Pressure Monitoring
Since high blood pressure can both cause and worsen kidney disease, regular monitoring is essential.
Stages of Diabetic Kidney Disease
Kidney disease generally develops gradually over several stages.
- 1. Early kidney changes – Slight increases in kidney filtration and small amounts of protein in the urine
- 2. Microalbuminuria – Detectable protein leakage begins
- 3. Moderate kidney damage – Filtration ability begins to decline
- 4. Severe kidney damage – Significant loss of kidney function
- 5. End-stage renal disease – Kidneys can no longer adequately filter waste
Early detection during the first stages offers the best opportunity to slow or prevent further damage.
Protecting Kidney Health
While diabetic nephropathy is a serious condition, many cases can be prevented or slowed through proper management.
Maintain Healthy Blood Sugar Levels
Keeping blood glucose within recommended ranges is one of the most important steps for protecting kidney function.
Strategies include:
- Monitoring blood glucose regularly
- Following a diabetes-friendly meal plan
- Taking medications or insulin as prescribed
- Attending regular medical appointments
Consistent glucose control reduces stress on the kidney’s filtering system.
Control Blood Pressure
Managing blood pressure is critical for slowing kidney damage.
Healthcare providers often recommend maintaining blood pressure below 130/80 mmHg for many patients with diabetes. Medications such as ACE inhibitors or ARBs are commonly prescribed because they help protect kidney function.
Follow a Kidney-Friendly Diet
Dietary adjustments can help reduce the workload on the kidneys.
Patients may benefit from:
- Reducing sodium intake
- Limiting highly processed foods
- Eating moderate amounts of protein
- Choosing fresh fruits and vegetables
- Staying properly hydrated
A registered dietitian can help design a personalized meal plan that supports both diabetes and kidney health.
Stay Physically Active
Regular physical activity supports healthy blood sugar levels, improves circulation, and helps control blood pressure.
The Centers for Disease Control and Prevention recommends that adults aim for at least 150 minutes of moderate-intensity exercise each week.
Avoid Smoking
Smoking damages blood vessels throughout the body, including those in the kidneys. Quitting smoking can significantly reduce the risk of kidney and cardiovascular complications.
Get Regular Kidney Screenings
Routine testing is one of the most effective ways to catch kidney disease early. Most diabetes care guidelines recommend annual testing for kidney function and urine protein levels.
These screenings allow healthcare providers to detect early changes and intervene before severe damage occurs.
Treatment Options for Advanced Kidney Disease
If diabetic nephropathy progresses to severe stages, additional treatments may be necessary.
These may include:
- Specialized medications to control blood pressure and reduce protein loss
- Dialysis, a treatment that filters waste from the blood when the kidneys cannot
- Kidney transplantation in cases of End-Stage Renal Disease
Early treatment and careful management can delay or prevent the need for these interventions.
Living With Diabetes and Protecting Your Kidneys
For individuals living with diabetes, protecting kidney health is a critical part of overall disease management. Although diabetic nephropathy is a serious condition, it is often preventable or manageable with early detection and proper care.
By maintaining healthy blood sugar levels, controlling blood pressure, adopting heart-healthy lifestyle habits, and working closely with healthcare providers, patients can significantly reduce their risk of developing kidney complications.
Taking proactive steps today can help preserve kidney function and support long-term health for years to come.
